An initial investigation of the role of depressive and anxious syndromes in Problematic Internet Use in adolescence and young adults
Vol.17,No.1(2023)
Depressive and anxious syndromes have been proposed as risk factors and as consequences of Problematic Internet Use (PIU). There has been no study relating affective symptoms in subjects with Problematic Internet Use and those with major depressive and anxious syndromes. In this study, three samples were collected: two from ambulatory clinical settings of the North Lisbon Hospital Centre (1. Centre for PIU and 2. Out-patient psychiatry consultation for adolescents and young adults) and a control group from Faculdade de Medicina da Universidade de Lisboa. Internet use profile and affective psychopathology were assessed and socio-demographic characteristics were controlled. The results revealed that both the PIU group and the clinical group presented significantly higher depression and anxiety scores than the control group while there was no significant difference between them. Also, Problematic Internet Users, similarly to the clinical group, tend to live in less functional families. We speculate that the similitude between samples and yet such different clinical presentations could be explained if Internet acted as a buffer to affective psychopathology. These findings warrant exploring the possibility of PIU as new (and generation biased) psychopathology of depressive or anxious states.
Problematic Internet Use; affective symptoms; anxiety; depression
Sofia Botelho de Sousa Paulino
Departamento de Psiquiatria e Saúde Mental, Hospital de Cascais, Dr. José de Almeida, Lisbon, Portugal
Sofia Paulino is a Psychiatrist at Departamento de Psiquiatria e Saúde Mental—Hospital de Cascais, Dr. José de Almeida, Portugal. She was Professor of Psychiatry between 2014 and 2020. Her research interests focus on adolescence, self-injurious and suicidal behaviors, temperament and new technologies.
Bárbara Mesquita
Departamento de Psiquiatria e Saúde Mental, Hospital de Cascais, Dr. José de Almeida, Lisbon, Portugal
Bárbara Mesquita is a Psychiatry resident at Departamento de Psiquiatria e Saúde Mental—Hospital de Cascais, Dr. José de Almeida, Portugal. Her main research interests are in addictive media use and their impact on mental health.
Ana M. Fraga
Departamento de Psiquiatria e Saúde Mental, Hospital de Cascais, Dr. José de Almeida, Lisbon, Portugal
Ana Margarida Fraga is a Psychiatry resident at Departamento de Psiquiatria e Saúde Mental—Hospital de Cascais, Dr. José de Almeida, Portugal. She is a PhD student in Neurosciences at the University of Porto. Her main research interests are in social media use among adolescents and their impact in mental health.
Hugo Gomes
Center for Psychology, University of Porto, Porto, Portugal
Hugo Gomes is a Fullbright Scholar and a Doctorate Researcher at the Center for Psychology at the University of Porto, and a PhD in applied psychology from the University of Minho, in collaboration with the Institute of Criminology, University of Cambridge. His main research interests are in research methods, developmental and life-course criminology, and experimental criminology. He was awarded the 2020’s Student Paper Award by the Division of Experimental Criminology of the American Society of Criminology (ASC).
Luís Madeira
Faculty of Medicine, University of Lisbon, Lisbon, Portugal
Luís Madeira is a Psychiatrist and the vice-president of Portuguese Society of Psychiatry. He holds a Master’s degree in Philosophy and a PhD in Medicine. He is Assistant Professor of Medical Ethics and Deontology and of Psychiatry at the Faculty of Medicine of the University of Lisbon. He is also a Psychotherapist with the Portuguese Society for Client-Centred Psychotherapy and Person-Centred Approach.
Aarseth, E., Bean, A. M., Boonen, H., Colder Carras, M., Coulson, M., Das, D., Deleuze, J., Dunkels, E., Edman, J., Ferguson, C. J., Haagsma, M. C., Hekmersson Bergmark, K., Hussain, Z., Jansz, J., Kardefelt-Winther, D., Kutner, L., Markey, P, Lundedal Nielsen, R. K., Prause, . . . Van Rooij, A. J. (2017). Scholars’ open debate paper on the World Health Organization ICD-11 Gaming Disorder proposal. Journal of Behavioral Addictions, 6(3), 267–270. https://doi.org/10.1556/2006.5.2016.088
Adiele, I., & Olatokun, W. (2014). Prevalence and determinants of Internet addiction among adolescents. Computers in Human Behavior, 31, 100–110. https://doi.org/10.1016/j.chb.2013.10.028
American Psychiatric Association (2013). Diagnostic and statistical manual of mental disorders (5th ed.). American Psychiatric Association.
Baek, Y. M., Bae, Y., & Jang, H. (2013). Social and parasocial relationships on social network sites and their differential relationships with users’ psychological well-being. Cyberpsychology, Behavior and Social Networking, 16(7), 512–517. https://doi.org/10.1089/cyber.2012.0510
Balconi, M., Venturella, I., & Finocchiaro, R. (2017). Evidences from rewarding system, FRN and P300 effect in Internet-addiction in young people. Brain Sciences, 7(7), Article 81. https://doi.org/10.3390/brainsci7070081
Bandura, A. (1991). Social cognitive theory of self-regulation. Organizational Behavior and Human Decision Processes, 50(2), 248–287. https://doi.org/10.1016/0749-5978(91)90022-l
Barry, C. T., Sidoti, C. L., Briggs, S. M., Reiter, S. R., & Lindsey, R. A. (2017). Adolescent social media use and mental health from adolescent and parent perspectives. Journal of Adolescence, 61(1), 1–11. https://doi.org/10.1016/j.adolescence.2017.08.005
Baxter, A. J., Scott, K. M., Vos, T., & Whiteford, H. A. (2012). Global prevalence of anxiety disorders: A systematic review and meta-regression. Psychological Medicine, 43(5), 897–910. https://doi.org/10.1017/s003329171200147x
Beck, A. T., Ward, C. H., Mendelson, M., Mock, J., & Erbaugh, J. (1961). An inventory for measuring depression. Archives of General Psychiatry, 4(6), 561–571. https://doi.org/10.1001/archpsyc.1961.01710120031004
Best, P., Manktelow, R., & Taylor, B. (2014). Online communication, social media and adolescent wellbeing: A systematic narrative review. Children and Youth Services Review, 41, 27–36. https://doi.org/10.1016/j.childyouth.2014.03.001
boyd, d. m., & Ellison, N. B. (2007). Social network sites: Definition, history, and scholarship. Journal of Computer-Mediated Communication, 13(1), 210–230. https://doi.org/10.1111/j.1083-6101.2007.00393.x
Brand, M., Young, K. S., & Laier, C. (2014). Prefrontal control and Internet addiction: A theoretical model and review of neuropsychological and neuroimaging findings. Frontiers in Human Neuroscience, 8, Article 375. https://doi.org/10.3389/fnhum.2014.00375
Brand, M., Young, K. S., Laier, C., Wölfling, K., & Potenza, M. N. (2016). Integrating psychological and neurobiological considerations regarding the development and maintenance of specific Internet-use disorders: An Interaction of Person-Affect-Cognition-Execution (I-PACE) model. Neuroscience & Biobehavioral Reviews, 71, 252–266. https://doi.org/10.1016/j.neubiorev.2016.08.033
Byles, J., Byrne, C., Boyle, M. H., & Offord, D. R. (1988). Ontario child health study: Reliability and validity of the General Functioning subscale of the McMaster Family Assessment Device. Family Process, 27(1), 97–104. https://doi.org/10.1111/j.1545-5300.1988.00097.x
Chou, H.-T. G., & Edge, N. (2012). “They are happier and having better lives than I am”: The impact of using Facebook on perceptions of others’ lives. Cyberpsychology, Behavior, and Social Networking, 15(2), 117–121. https://doi.org/10.1089/cyber.2011.0324
Cudo, A., Torój, M., Misiuro, T., & Griffiths, M. D. (2020). Problematic Facebook use and problematic video gaming among female and male gamers. Cyberpsychology, Behavior, and Social Networking, 23(2), 126–133. https://doi.org/10.1089/cyber.2019.0252
Davis, R. A. (2001). A cognitive-behavioral model of pathological Internet use. Computers in Human Behavior, 17(2), 187–195. https://doi.org/10.1016/S0747-5632(00)00041-8
Ding, W.-n., Sun, J.-h., Sun, Y.-w., Chen, X., Zhou, Y., Zhuang, Z.-g., Li, L., Zhang, Y., Xu, J.-r., & Du, Y.-s. (2014). Trait impulsivity and impaired prefrontal impulse inhibition function in adolescents with Internet gaming addiction revealed by a go/no-go fMRI study. Behavioral and Brain Functions, 10(1), Article 20. https://doi.org/10.1186/1744-9081-10-20
Ding, W.-n., Sun, J.-h., Sun, Y.-w., Zhou, Y., Li, L., Xu, J.-r., & Du, Y.-s. (2013). Altered default network resting-state functional connectivity in adolescents with Internet gaming addiction. PLoS One, 8(3), Article e59902. https://doi.org/10.1371/journal.pone.0059902
Durkee, T., Kaess, M., Carli, V., Parzer, P., Wasserman, C., Floderus, B., Apter, A., Balazs, J., Barzilay, S., Bobes, J., Brunner, R., Corcoran, P., Cosman, D., Cotter, P., Despalins, R., Graber, N., Guillemin, F., Haring, C., Kahn, J.-P, . . . Wasserman, D. (2012). Prevalence of pathological Internet use among adolescents in Europe: Demographic and social factors: Pathological Internet use among adolescents. Addiction, 107(12), 2210–2222. https://doi.org/10.1111/j.1360-0443.2012.03946.x
Ellison, N. B., Steinfield, C., & Lampe, C. (2007). The benefits of Facebook “friends:” Social capital and college students’ use of online social network sites. Journal of Computer-Mediated Communication, 12(4), 1143–1168. https://doi.org/10.1111/j.1083-6101.2007.00367.x
Epstein, N. B., Baldwin, L. M., & Bishop, D. S. (1983). The McMaster Family Assessment Device. Journal of Marital and Family Therapy, 9(2), 171–180. https://doi.org/10.1111/j.1752-0606.1983.tb01497.x
Ferrari, A. J., Somerville, A. J., Baxter, A. J., Norman, R., Patten, S. B., Vos, T., & Whiteford, H. A. (2013). Global variation in the prevalence and incidence of major depressive disorder: A systematic review of the epidemiological literature. Psychological Medicine, 43(3), 471–481. https://doi.org/10.1017/s0033291712001511
Gámez-Guadix, M. (2014). Depressive symptoms and problematic Internet use among adolescents: Analysis of the longitudinal relationships from the cognitive-behavioral model. Cyberpsychology, Behavior and Social Networking, 17(11), 714–719. https://doi.org/10.1089/cyber.2014.0226
Gómez, P., Rial, A., Braña, T., Golpe, S., & Varela, J. (2017). Screening of problematic Internet use among Spanish adolescents: Prevalence and related variables. Cyberpsychology, Behavior, and Social Networking, 20(4), 259–267. https://doi.org/10.1089/cyber.2016.0262
González-Bueso, V., Santamaría, J. J., Fernández, D., Merino, L., Montero, E., & Ribas, J. (2018). Association between Internet gaming disorder or pathological video-game use and comorbid psychopathology: A comprehensive review. International Journal of Environmental Research and Public Health, 15(4), Article 668. https://doi.org/10.3390/ijerph15040668
Gorenstein, C., Andrade, L., Filho, A. H. G. V., Tung, T. C., & Artes, R. (1999). Psychometric properties of the Portuguese version of the Beck Depression Inventory on Brazilian college students. Journal of Clinical Psychology, 55(5), 553–562. https://doi.org/10.1002/(sici)1097-4679(199905)55:5<553::aid-jclp3>3.0.co;2-d
Griffiths, M. D. (1996). Behavioural addiction: An issue for everybody? Employee Counselling Today, 8(3), 19–25. https://doi.org/10.1108/13665629610116872
Griffiths, M. D. (2004). Does Internet and computer “addiction” exist? Some case study evidence. CyberPsychology & Behavior, 3(2), 211–218. https://doi.org/10.1089/109493100316067
Griffiths, M. D. (2005). A “component” model of addiction within a biopsychosocial framework. Journal of Substance Use, 10(4), 191–197. https://doi.org/10.1080/14659890500114359
Guo, Y., Li, Y., & Ito, N. (2014). Exploring the predicted effect of social networking site use on perceived social capital and psychological well-being of Chinese international students in Japan. Cyberpsychology, Behavior, and Social Networking, 17(1), 52–58. https://doi.org/10.1089/cyber.2012.0537
Halbrook, Y. J., O’Donnell, A. T., & Msetfi, R. M. (2019). When and how video games can be good: A review of the positive effects of video games on well-being. Perspectives on Psychological Science, 14(6), 1096–1104. https://doi.org/10.1177/1745691619863807
Hawi, N. S., Samaha, M., & Griffiths, M. D. (2018). Internet gaming disorder in Lebanon: Relationships with age, sleep habits, and academic achievement. Journal of Behavioral Addictions, 7(1), 70–78. https://doi.org/10.1556/2006.7.2018.16
Hirschfeld, R. M. A. (2001). The comorbidity of major depression and anxiety disorders: Recognition and management in primary care. Primary Care Companion to the Journal of Clinical Psychiatry, 3(6), 244–254. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC181193/
Hong, S.-B., Kim, J.-W., Choi, E.-J., Kim, H.-H., Suh, J.-E., Kim, C.-D., Klauser, P., Whittle, S., Yűcel, M., Pantelis, C., & Yi, S.-H. (2013). Reduced orbitofrontal cortical thickness in male adolescents with Internet addiction. Behavioral and Brain Functions, 9(1), Article 11. https://doi.org/10.1186/1744-9081-9-11
Hong, S.-B., Zalesky, A., Cocchi, L., Fornito, A., Choi, E.-J., Kim, H.-H., Suh, J.-E., Kim, C.-D., Kim, J.-W., & Yi, S.-H. (2013). Decreased functional brain connectivity in adolescents with Internet addiction. PLoS One, 8(2), Article e57831. https://doi.org/10.1371/journal.pone.0057831
Jin, B. (2013). How lonely people use and perceive Facebook. Computers in Human Behavior, 29(6), 2463–2470. https://doi.org/10.1016/j.chb.2013.05.034
Kardefelt-Winther, D. (2014). A conceptual and methodological critique of Internet addiction research: Towards a model of compensatory Internet use. Computers in Human Behavior, 31, 351–354. https://doi.org/10.1016/j.chb.2013.10.059
Kardefelt‐Winther, D., Heeren, A., Schimmenti, A., van Rooij, A., Maurage, P., Carras, M., Edman, J., Blaszczynski, A., Khazaal, Y., & Billieux, J. (2017). How can we conceptualize behavioural addiction without pathologizing common behaviours? Addiction, 112(10), 1709–1715. https://doi.org/10.1111/add.13763
Kircaburun, K., & Griffiths, M. D. (2018). The dark side of Internet: Preliminary evidence for the associations of dark personality traits with specific online activities and problematic Internet use. Journal of Behavioral Addictions, 7(4), 993–1003. https://doi.org/10.1556/2006.7.2018.109
Kirmayer, L. J., Raikhel, E., & Rahimi, S. (2013). Cultures of the Internet: Identity, community and mental health. Transcultural Psychiatry, 50(2), 165–191. https://doi.org/10.1177/1363461513490626
Kross, E., Verduyn, P., Demiralp, E., Park, J., Lee, D. S., Lin, N., Shablack, H., Jonides, J., & Ybarra, O. (2013). Facebook use predicts declines in subjective well-being in young adults. PLoS One, 8(8), Article e69841. https://doi.org/10.1371/journal.pone.0069841
Laconi, S., Rodgers, R. F., & Chabrol, H. (2014). The measurement of Internet addiction: A critical review of existing scales and their psychometric properties. Computers in Human Behavior, 41, 190–202. https://doi.org/10.1016/j.chb.2014.09.026
Lam, L. T. (2014). Risk factors of Internet addiction and the health effect of Internet addiction on adolescents: A systematic review of longitudinal and prospective studies. Current Psychiatry Reports, 16(11), Article 508. https://doi.org/10.1007/s11920-014-0508-2
LaRose, R., Lin, C. A., & Eastin, M. S. (2003). Unregulated Internet usage: Addiction, habit, or deficient self-regulation? Media Psychology, 5(3), 225–253. https://doi.org/10.1207/s1532785xmep0503_01
Lee, K.-T., Noh, M.-J., & Koo, D.-M. (2013). Lonely people are no longer lonely on social networking sites: The mediating role of self-disclosure and social support. Cyberpsychology, Behavior and Social Networking, 16(6), 413–418. https://doi.org/10.1089/cyber.2012.0553
Lemenager, T., Hoffmann, S., Dieter, J., Reinhard, I., Mann, K., & Kiefer, F. (2018). The links between healthy, problematic, and addicted Internet use regarding comorbidities and self-concept-related characteristics. Journal of Behavioral Addictions, 7(1), 31–43. https://doi.org/10.1556/2006.7.2018.13
Li, C., Dang, J., Zhang, X., Zhang, Q., & Guo, J. (2014). Internet addiction among Chinese adolescents: The effect of parental behavior and self-control. Computers in Human Behavior, 41, 1–7. https://doi.org/10.1016/j.chb.2014.09.001
Manago, A. M., Taylor, T., & Greenfield, P. M. (2012). Me and my 400 friends: The anatomy of college students’ Facebook networks, their communication patterns, and well-being. Developmental Psychology, 48(2), 369–380. https://doi.org/10.1037/a0026338
Marroquín, B. (2011). Interpersonal emotion regulation as a mechanism of social support in depression. Clinical Psychology Review, 31(8), 1276–1290. https://doi.org/10.1016/j.cpr.2011.09.005
Moon, S. J., Hwang, J. S., Kim, J. Y., Shin, A. L., Bae, S. M., & Kim, J. W. (2018). Psychometric properties of the Internet Addiction Test: A systematic review and meta-analysis. Cyberpsychology, Behavior, and Social Networking, 21(8), 473–484. https://doi.org/10.1089/cyber.2018.0154
Moreno, M. A., Jelenchick, L. A., & Breland, D. J. (2015). Exploring depression and problematic Internet use among college females: A multisite study. Computers in Human Behavior, 49, 601–607. https://doi.org/10.1016/j.chb.2015.03.033
Müller, K. W., Beutel, M. E., Dreier, M., & Wölfling, K. (2019). A clinical evaluation of the DSM-5 criteria for Internet gaming disorder and a pilot study on their applicability to further Internet-related disorders. Journal of Behavioral Addictions, 8(1), 16–24. https://doi.org/10.1556/2006.7.2018.140
Oh, H. J., Ozkaya, E., & LaRose, R. (2014). How does online social networking enhance life satisfaction? The relationships among online supportive interaction, affect, perceived social support, sense of community, and life satisfaction. Computers in Human Behavior, 30, 69–78. https://doi.org/10.1016/j.chb.2013.07.053
Oing, T., & Prescott, J. (2018). Implementations of virtual reality for anxiety-related disorders: Systematic review. JMIR Serious Games, 6(4), Article e10965. https://doi.org/10.2196/10965
Pais-Ribeiro, J., Silva, I., Ferreira, T., Martins, A., Meneses, R., & Baltar, M. (2007). Validation study of a Portuguese version of the Hospital Anxiety and Depression Scale. Psychology, Health & Medicine, 12(2), 225–237. https://doi.org/10.1080/13548500500524088
Park, S., Hong, K.-E. M., Park, E. J., Ha, K. S., & Yoo, H. J. (2013). The association between problematic Internet use and depression, suicidal ideation and bipolar disorder symptoms in Korean adolescents. The Australian and New Zealand Journal of Psychiatry, 47(2), 153–159. https://doi.org/10.1177/0004867412463613
Park, S. M., Park, Y. A., Lee, H. W., Jung, H. Y., Lee, J.-Y., & Choi, J.-S. (2013). The effects of behavioral inhibition/approach system as predictors of Internet addiction in adolescents. Personality and Individual Differences, 54(1), 7–11. https://doi.org/10.1016/j.paid.2012.07.033
Pontes, H. M. (2017). Investigating the differential effects of social networking site addiction and Internet gaming disorder on psychological health. Journal of Behavioral Addictions, 6(4), 601–610. https://doi.org/10.1556/2006.6.2017.075
Pontes, H. M., Patrão, I. M., & Griffiths, M. D. (2014). Portuguese validation of the Internet Addiction Test: An empirical study. Journal of Behavioral Addictions, 3(2), 107–114. https://doi.org/10.1556/jba.3.2014.2.4
Rosenquist, J. N., Fowler, J. H., & Christakis, N. A. (2011). Social network determinants of depression. Molecular Psychiatry, 16(3), 273–281. https://doi.org/10.1038/mp.2010.13
Shapiro, L. A. S., & Margolin, G. (2014). Growing up wired: Social networking sites and adolescent psychosocial development. Clinical Child and Family Psychology Review, 17(1), 1–18. https://doi.org/10.1007/s10567-013-0135-1
Snaith, R. P. (2003). The Hospital Anxiety and Depression Scale. Health and Quality of Life Outcomes, 1(1), Article 29. https://doi.org/10.1186/1477-7525-1-29
Starcevic, V., & Aboujaoude, E. (2017). Internet addiction: Reappraisal of an increasingly inadequate concept. CNS Spectrums, 22(1), 7–13. https://doi.org/10.1017/s1092852915000863
Steger, M. F., & Kashdan, T. B. (2009). Depression and everyday social activity, belonging, and well-being. Journal of Counseling Psychology, 56(2), 289–300. https://doi.org/10.1037/a0015416
Strong, C., Lee, C.-T., Chao, L.-H., Lin, C.-Y., & Tsai, M.-C. (2018). Adolescent Internet use, social integration, and depressive symptoms: Analysis from a longitudinal cohort survey. Journal of Developmental & Behavioral Pediatrics, 39(4), 318–324. https://doi.org/10.1097/dbp.0000000000000553
Tan, Y., Chen, Y., Lu, Y., & Li, L. (2016). Exploring associations between problematic Internet use, depressive symptoms and sleep disturbance among southern Chinese adolescents. International Journal of Environmental Research and Public Health, 13(3), Article 313. https://doi.org/10.3390/ijerph13030313
Valkenburg, P. M., & Peter, J. (2009). The effects of instant messaging on the quality of adolescents’ existing friendships: A longitudinal study. Journal of Communication, 59(1), 79–97. https://doi.org/10.1111/j.1460-2466.2008.01405.x
van den Eijnden, R. J. J. M., Meerkerk, G.-J., Vermulst, A. A., Spijkerman, R., & Engels, R. C. M. E. (2008). Online communication, compulsive Internet use, and psychosocial well-being among adolescents: A longitudinal study. Developmental Psychology, 44(3), 655–665. https://doi.org/10.1037/0012-1649.44.3.655
Wartberg, L., Kammerl, R., Rosenkranz, M., Hirschhäuser, L., Hein, S., Schwinge, C., Petersen, K.-U., & Thomasius, R. (2014). The interdependence of family functioning and problematic Internet use in a representative quota sample of adolescents. Cyberpsychology, Behavior, and Social Networking, 17(1), 14–18. https://doi.org/10.1089/cyber.2012.0494
Wartberg, L., Kriston, L., & Thomasius, R. (2020). Internet gaming disorder and problematic social media use in a representative sample of German adolescents: Prevalence estimates, comorbid depressive symptoms and related psychosocial aspects. Computers in Human Behavior, 103, 31–36. https://doi.org/10.1016/j.chb.2019.09.014
Weinstein, A., Dorani, D., Elhadif, R., Bukovza, Y., Yarmulnik, A., & Dannon, P. (2015). Internet addiction is associated with social anxiety in young adults. Annals of Clinical Psychiatry: Official Journal of the American Academy of Clinical Psychiatrists, 27(1), 4–9. https://pubmed.ncbi.nlm.nih.gov/25696775/
Wilson, R. E., Gosling, S. D., & Graham, L. T. (2012). A review of Facebook research in the social sciences. Perspectives on Psychological Science: A Journal of the Association for Psychological Science, 7(3), 203–220. https://doi.org/10.1177/1745691612442904
Wu, C. S. T., Wong, H. T., Yu, K. F., Fok, K. W., Yeung, S. M., Lam, C. H., & Liu, K. M. (2016). Parenting approaches, family functionality, and Internet addiction among Hong Kong adolescents. BMC Pediatrics, 16(1), Article 130. https://doi.org/10.1186/s12887-016-0666-y
Young, K. S. (1998). Internet addiction: The emergence of a new clinical disorder. CyberPsychology & Behavior, 1(3), 237–244. https://doi.org/10.1089/cpb.1998.1.237
Yu, J. J., Kim, H., & Hay, I. (2013). Understanding adolescents’ problematic Internet use from a social/cognitive and addiction research framework. Computers in Human Behavior, 29(6), 2682–2689. https://doi.org/10.1016/j.chb.2013.06.045
Zhong, X., Zu, S., Sha, S., Tao, R., Zhao, C., Yang, F., Li, M., & Sha, P. (2011). The effect of a family-based intervention model on Internet-addicted Chinese adolescents. Social Behavior and Personality: An International Journal, 39(8), 1021–1034. https://doi.org/10.2224/sbp.2011.39.8.1021
Zhou, N., Cao, H., Li, X., Zhang, J., Yao, Y., Geng, X., Lin, X., Hou, S., Liu, F., Chen, X., & Fang, X. (2018). Internet addiction, problematic Internet use, nonproblematic Internet use among Chinese adolescents: Individual, parental, peer, and sociodemographic correlates. Psychology of Addictive Behaviors, 32(3), 365–372. https://doi.org/10.1037/adb0000358
Zigmond, A. S., & Snaith, R. P. (1983). The Hospital Anxiety and Depression Scale. Acta Psychiatrica Scandinavica, 67(6), 361–370. https://doi.org/10.1111/j.1600-0447.1983.tb09716.x
Authors’ Contribution
Sofia Paulino: conceptualization, data curation, formal analysis, project administration, writing—original draft, writing—review & editing. Bárbara Mesquita: investigation, project administration, writing—original draft, writing—review & editing. Ana Margarida Fraga: investigation, writing—review & editing. Hugo Gomes: methodology. Luís Madeira: conceptualization, project administration, supervision.
Editorial Record
First submission received:
April 6, 2020
Revisions received:
April 4, 2021
September 14, 2022
Accepted for publication:
December 5, 2022
Editor in charge:
David Smahel
Introduction
Internet emerges in this digital era as an useful instrument of work, leisure and culture, and the multiple virtual alternatives offer a sense of affection, inclusion and self-efficacy that inevitably attract a large part of the population (Kirmayer et al., 2013). Given this globalized online immersion of the population, the benefits are obvious and objective, but the risks and consequences are also critical to analyse (Kircaburun & Griffiths, 2018; Lam, 2014; Lemenager et al., 2018). Despite being an extremely popular topic of the moment, research remains inconsistent, therefore it is not yet possible to define consistent guidelines for an appropriate use (Griffiths, 2004; Laconi et al., 2014; Starcevic & Aboujaoude, 2017).
The dysfunctional use of the Internet is being conceptualized as Problematic Internet Use (PIU) and described as a persistent involvement in non-essential online activities that results in negative emotional and social consequences (Barry et al., 2017). Problematic Internet users seem of be primarily adolescents and young adults who, depending on the use of the Internet, left alternative routines, reduced family coexistence, reduced offline social contacts, and directly or indirectly compromised their academic or occupational obligations (Gómez et al., 2017; Young, 1998).
Numerous authors proposed different models to explain this inappropriate use of the Internet that implies negative consequences for the self. In line with the cognitive-behavioral model of Problematic Internet Use, maladaptative cognitions about the self (i.e., perfectionism discrepancies) and the world (i.e., social hopelessness) have primary importance in the development of a preference for online interaction (Davis, 2001). In line with the addiction model, executive control processes are particularly reduced in individuals with Problematic Internet Use as in substance use disorders (Brand et al., 2014).
Griffiths’ component model of behavioural addiction unifies the symptoms of behavioural addictions. More precisely, Griffiths postulates that five behavioural addiction criteria occur in all behavioural addictions (Griffiths, 1996, 2005), namely salience (online activity is so central in life that it interferes with basic needs like sleep, food or hygiene), mood modifications (online activity is used to achieve a positive change in mood serving as a coping strategy to manage negative emotions), tolerance (more and more hours are needed to achieve the same mood swing), withdrawal (feelings of tiredness and irritability, sometimes of severe dysphoria, when the Internet is inaccessible) and conflict (aggressive reactions when restriction is imposed, often in breach with habitual personality traits; González-Bueso et al., 2018; Müller et al., 2019; Yu et al., 2013). According to Griffiths’ model, when only some symptoms are present, this can indicate problematic behaviour (Griffiths, 1996, 2005).
Most authors separate generalized Internet use disorder from specific Internet use disorders like problematic gaming, problematic social media use, problematic pornography use, etc. (Brand et al., 2016; Cudo et al., 2020; Pontes, 2017; Wartberg et al., 2020). This research aims to evaluate generalized Internet use and therefore does not specify into its different groups.
Nevertheless, it is important to mention specifically Internet Gaming Disorder (IGD) as it is the only condition that has been acknowledged in the Internet Classification of Diseases (ICD) and is under investigation in the DSM-5. The appendix III of the DSM-5 includes, also as criteria, preoccupation or obsession, loss of control, loss of interest, continued overuse, deceiving, escape from negative feelings and functional impairment (APA, 2013, p. 795). Recent research suggest that IGD and PIU are different conditions or that IGD is a subtype of PIU.
Therefore, the criteria proposed by Griffiths and by the DSM are mentioned here to help the identification and analysis (not the formal diagnosis as there are not yet consistent criteria proposed specifically for PIU.
Nevertheless these criteria appear to be supported by neurobiological research that considers PIU as a disorder that affects reward and impulsive/inhibition brain pathways, as it is unambiguous that Internet is able to provide, in most situation, more intense stimuli and stronger sensations than every day’s real life (Balconi et al., 2017; Ding et al., 2013, 2014; Hong, Kim, et al., 2013; Hong, Zalesky, et al., 2013; S. Park et al., 2013; S. M. Park et al., 2013). This possible explanation is not sufficient to understand why some users engage in a dysfunctional use and others don’t.
In recent years, concerns have been raised regarding links between affective disorders, namely depressive and anxious major syndromes, and PIU (Gámez-Guadix, 2014; Strong et al., 2018).
Affective disorders such as depression and anxiety have been shown to have bidirectional interactions with the social environment that influence the path of illness onset and maintenance (Marroquín, 2011). In the global population, depression and anxiety have an approximate prevalence of 4.7% and 7.3%, respectively (Baxter et al., 2012; Ferrari et al., 2013; Lam, 2014). These disorders have high levels of comorbidity, impact the quality of social relationships and are very common mental health issues, with an onset usually during adolescence (Hirschfeld, 2001; Rosenquist et al., 2011; Steger & Kashdan, 2009).
Considerable disagreement exists as to associations that Internet use may have with these two disorders (Best et al., 2014; Shapiro & Margolin, 2014). In this social perspective, on one hand, Internet use may protect from mental illness, as it supports, enables, and extends social interaction (boyd & Ellison, 2007; Ellison et al., 2007; Wilson et al., 2012) giving a sense of belonging and of social connectedness (Baek et al., 2013; Guo et al., 2014; Jin, 2013; Lee et al., 2013; Manago et al., 2012; Oh et al., 2014). On the other hand, there are many opportunities for miscommunications and mismanaged expectations, and maladaptive tendencies can be exaggerated, leading to a greater sense of isolation (Baek et al., 2013; Best et al., 2014; Steger & Kashdan, 2009). Indeed, the literature, in this field, is divided between studies that consider that anxious and depressive symptoms promote the dysfunctional use of the Internet, and others that defend the opposite: it is the PIU that promotes angodepressive symptoms (Hawi et al., 2018; Hirschfeld, 2001; S. Park et al., 2013; Tan et al., 2016; Weinstein et al., 2015).
We put forward as a general goal of the present investigation the analysis of the relationship between depressive and anxious symptoms and Internet use.
H1: Problematic Internet Users would have some affective symptomatology, but different from those with major depressive or anxious symptoms.
H2: Problematic Internet Users would have symptoms resembling those of people with diagnosed affective disorders, suggesting PIU would be a new manifestation of disorders already known.
H3: Problematic Internet Users would have no other significant comorbid psychopathology, which would be in line with the idea that PIU is an independent nosologic entity by exclusion of the others (Aarseth et al., 2017; Kardefelt-Winther, 2014; Kardefelt‐Winther et al., 2017; Young, 1998).
Lastly, we aimed to determine the correlation between family functioning, angodepressive symptoms and Internet use.
Methods
Design and Subjects
A correlation and comparative naturalistic study was designed to evaluate the interaction between PIU and anxiety and depression. Three samples were collected from July 2018 to December 2019, giving a total of 79 adolescents.
A sample of 17 Problematic Internet Users diagnosed according to the DSM-5 appendix III proposed criteria (Müller et al., 2019) was collected from the PIU Nucleus of the Department of Psychiatry and Mental Health of Santa Maria University Hospital. This Unit, a pioneer in Portugal since 2014, works with an outpatient program for adolescents and young adults aged 15 years-old or over who consider (or more often, whose family considers) that Internet has become a problem interfering with normal functioning.
A sample of 30 adolescents and young adults with anxious and depressive syndromes diagnosed according to DSM-5 criteria was collected from the Adolescent and Young Adults Unit of the Department of Psychiatry and Mental Health of Santa Maria University Hospital.
A third group of 32 adolescents and young adults (control group) was collected from the Medical School of Santa Maria University Hospital.
Socio-demographic and Internet use profile information was collected at admission with a standardized interview. Diagnosis was established with clinical evaluation by an experienced psychiatrist. Other diagnoses were established or excluded using Mini Neuropsychiatric Interview.
All the subjects included in the study participated voluntarily and gave informed consent. The study was approved by the ethics committee of Santa Maria Hospital.
Instruments
Patients were assessed with the following instruments.
Internet Addiction Test (IAT)
IAT is a self-administered questionnaire developed by Kimberly Young to measure Internet use severity. Information is gathered through 20 self-reported items, with dysfunctional use of the Internet being defined as meeting five of seven criteria over a six-month period: obsession with the Internet, increasingly longer periods spent on the Internet, having time management problems, repeated attempts to reduce Internet use, environmental distress, deception regarding time spent online, and mood modification through Internet use. IAT appears to be the most consistent and reliable measure tool for Internet use developed so far (Moon et al., 2018). A Portuguese version of the IAT was developed and validated in a Portuguese sample and showed good psychometric properties (Pontes et al., 2014). The present study showed good internal consistency (α = .92).
Beck Depression Inventory (BDI)
BDI is a self-administered questionnaire developed by Aaron T. Beck to measure depression severity. In its current version, the BDI is designed for individuals aged 13 and over and is composed of 21 multiple-choice items relating to symptoms of depression such as hopelessness and irritability, cognitions such as guilt or feelings of being punished, as well as physical symptoms such as fatigue, weight loss, and lack of interest in sex. It has high internal consistency and high content validity (Beck et al., 1961). A Portuguese version was developed and validated with good psychometric properties (Gorenstein et al., 1999). In the present study, BDI presented very good internal consistency (α = .95).
Hospital Anxiety and Depression Scale (HADS)
HADS was originally developed by Zigmond and Snaith to determine levels of anxiety and depression while avoiding relying on symptoms of these conditions that are also common somatic symptoms of illness (for example, fatigue and insomnia or hypersomnia). It is a fourteen-item scale that generates ordinal data: seven of the items relate to anxiety and seven relate to depression (Zigmond & Snaith, 1983). The term “hospital” in its designation suggests that it is only valid in such a setting, but many studies conducted throughout the world have confirmed its validity in ambulatory settings (Snaith, 2003). A Portuguese version was developed and validated (Pais-Ribeiro et al., 2007). In this study, the HADS presented a good Cronbach’s alpha for the Anxiety scale (α = .91) and acceptable scores for the Depression scale (α = .86).
Family Assessment Device—General Functioning
The General Functioning 12-item subscale of the McMaster Family Assessment Device (Epstein et al., 1983) has been validated as a single index measure to assess family functioning. This subscale has virtually equivalent psychometric properties and is able to identify almost all of the same families who had healthy or unhealthy levels of functioning as the full scale. It is a quick and effective tool to assess overall functioning of families (Byles et al., 1988). The present study showed very good internal consistency (α = .98).
Statistical Analysis
Statistical analyses were developed using SPSS v24 software (IBM SPSS, Chicago, IL). The comparisons between the three groups regarding categorical variables were carried out using Chi-Square tests. As for mean comparisons, one-way ANOVA with Least Significant Difference (LSD) post-hoc tests were used when the normality assumption was fulfilled for all groups, otherwise the Kruskal-Wallis nonparametric tests were used.
As for mean comparisons, one-way ANOVA with Least Significant Difference (LSD) post-hoc tests were used when the normality assumption was fulfilled for all groups, otherwise the Kruskal-Wallis nonparametric tests with Dunn’s post-hoc pairwise comparisons were used.
Results
Sociodemographic data
Sex
From the three groups under analysis, the PIU group included 76.5% males (n = 13), the clinical group presented 46.7% males (n = 14) and the control group presented 40.6% males (n = 13). According to the Chi-Square test, despite the PIU group showing a larger proportion of male participants, no statistically significant different proportions of female and male participants were found, χ2(2) = 6.01, p = .050, Cramer’s V = .28.
Age
Within the three groups under analysis, the PIU group included a mean age of 19.65 years (SD = 2.76, Min = 15, Max = 32), the clinical group presented a mean age of 18.83 (SD = 3.31), and the control group presented a mean age 19.84 years (SD = 1.63). According to the Kruskal-Wallis test, participants in the clinical group were significantly younger than the participants in the control group and the difference was statistically significant, c2kw(2) = 6.36, Z = 14.56, p = .005, h2 = .10. No significant differences were found between PIU and the clinical group (z = 7.29, p = .872) or between PIU and the control group (z = −7.27, p = .859).
Academic Status
Most participants in PIU group were in high school (64.7%, n = 11), with only 2 participants in primary school (11.8%) and 4 in university (23.5%). Similarly, most participants in the clinical group were in high school (62.1%, n = 18) with only 6 in primary school (20.7%) and 5 (17.2%) in university. On the other hand, all the participants in the control group were University students.
Concerning academic performance, most PIU participants presented at least one academic retention in the past (64.7%, n = 11) against 36.7% (n = 11) of the clinical group participants and 21.9% (n = 7) of the control group participations. Chi-square test showed a statistically significant difference between the PIU group and the control group, χ2(2) = 8.77, p = .001, Cramer’s V = .37.
Nuclear Family
Most of the PIU group participants lived in a single-parent family (all with their mothers; 35.3%, n = 6) or in a reconstructed family (29.4%, n = 5). The majority of the clinical group participants lived with both parents (46.7%, n = 14) or in a single-parent household with their mothers (30.0%, n = 9). The control group presented 56.3% of participants living with both parents (n = 18), followed by 28.1% (n = 9) living only with their mothers.
Social Support
The majority of the PIU and the clinical group participants denied having a romantic relationship (76.5%, n = 13 and 53.3%, n = 16 respectively). On the other hand, the majority of controls reported being in a current relationship (71.9%, n = 23). Chi-square analysis showed a statistically significant difference between the PIU group when compared with the control group, χ2(2) = 10.93, p = .004, Cramer’s V = .37.
Concerning perceived friendship support, most people in the three groups reported having only a few friends (PIU group: 69.2%, n = 9; clinical group: 76.9%, n = 20; and control group 83.3%, n = 15). Only 23.5% of the PIU group and 17.2% of the clinical group reported not having any friends, against none of the control group.
Socioeconomic Status
The majority of the three groups participants lived in an urban environment (PIU group: 100%, n = 17; clinical group: 76.7%, n = 23; control group: 96.9%, n = 31) and belonged to a middle economic class (PIU group: 64.7%, n = 11; clinical group: 78.6%, n = 22; 90.6%, n = 29). Four (23.5%) participants of the PIU group, 5 (17.9%) of the control group and none of the control group reported belonging to a low economic class.
Internet Use Profile
Age of Beginning Internet Use
As for the comparison of Internet use profile between groups, our results showed a mean age of 9.88 years (SD = 2.80) for the PIU group, 9.79 years (SD = 2.88) for the clinical group and 11.81 years (SD = 1.94) for the control group. According to the Kruskal-Wallis test, there were significant differences, c2kw(2) = 9.63, p = .008, h2 = .13. Pairwise comparisons revealed that PIU group (z = −16.84, p = .011) and clinical group (z = 15.31, p = .007) participants started using the Internet at significantly younger ages than controls. No significant differences were found between PIU and clinical groups (z = −1.53, p = .821).
Leisure Versus Study Internet Time
Descriptive analysis shows that the PIU group participants use the Internet for leisure for a mean of 10.15 (SD = 4.14) hours per day, the clinical group for a mean of 6.88 (SD = 3.95), and the control group for a mean of 3.87 (SD = 1.76). The Kruskal-Wallis analysis showed statistically significant differences between groups, c2kw(2) = 25.59, p < .001, h2 = .35: post hoc test revealed a statistically significant difference between the time used by the PIU group participants when compared with the clinical group (z = −17.63, p = .002) and with the control group (z = 32.361, p < .001). Moreover, the clinical group reported a marginally significant higher use of the Internet for leisure than the control group (z = 14.73, p = .027).
For study, the PIU group participants reported a mean of 1.41 (SD = 1.91) hours per day, the clinical group a mean of 1.84 (SD = 2.05), and the control group a mean of 3.71 (SD = 2.25). The Kruskal-Wallis test revealed also statistically significant differences between the groups, c2kw(2) = 16.07, p < .001, h2 = .21. Pairwise comparisons showed that the control group reported a higher mean hours of Internet study than the PIU group (z = −23.42, p = .001) and the clinical group (z = 18.31, p = .001). No significant differences were found between PIU and the Clinical group (z = −5.11, p = .449).
Table 1. Descriptive Analysis of Internet Use Profile Data.
|
|
PIU |
Clinical |
Control |
Test |
|||
|
|
M |
SD |
M |
SD |
M |
SD |
|
|
Onset (years) |
9.88a |
2.80 |
9.79a |
2.88 |
11.81b |
1.94 |
c2kw(2) = 9.63, p = .008 |
|
Leisure (hours/day) |
10.15a |
4.14 |
6.88b |
3.95 |
3.87b |
1.76 |
c2kw(2) = 25.59, p < .001 |
|
Study (hours/day) |
1.41a |
1.91 |
1.84a |
2.05 |
3.71b |
2.25 |
c2kw(2) = 16.07, p < .001 |
|
Note. The subscript letters next to the mean scores represent the results of the post hoc pairwise comparison tests for the comparison between groups’ proportions at the .05 level; if the letters in the same row are different the proportions differ significantly; if the letters in the same row are equal the differences in proportions are not statistically significant. |
|||||||
Internet Provider
Descriptive analyses show that, for most of the participants, Internet is payed for by their family. Only 1 participant in the PIU group and 2 participants in the control group pay Internet on their own.
Preferred Internet Activities
Most participants in PIU and clinical groups reported, in order of importance, video games as the most important activity (70.6%, n = 12 and 34.5%, n = 10 respectively), multimedia as the second (64.7%, n = 11 and 44.8%, n = 13), and email/chat as the third (35.3%, n = 6 and 37.9%, n = 11). In the control group, most participants reported, in order of importance, social networks as the first and third most important activity (38.7%, n = 12; 25.8%, n = 8) and multimedia as the second (51.6%, n = 16; Table 2).
Table 2. Descriptive Analysis of the Most Important Activities in the Internet.
|
First most important Internet activities |
Second most important Internet activities |
Third most important Internet activities |
|||||||
|
|
PIU (n = 17) |
Clinical (n = 29) |
Control (n = 31) |
PIU (n = 17) |
Clinical (n = 29) |
Control (n = 31) |
PIU (n = 17) |
Clinical (n = 29) |
Control (n = 31) |
|
Video games |
70.60% |
34.50% |
9.70% |
11.80% |
17.20% |
6.50% |
— |
6.90% |
12.90% |
|
Social media |
17.60% |
31.00% |
38.70% |
11.80% |
24.10% |
19.40% |
23.50% |
17.20% |
25.80% |
|
Multimedia |
11.80% |
13.80% |
22.60% |
64.70% |
44.80% |
51.60% |
11.80% |
13.80% |
19.40% |
|
Email / chat |
— |
13.80% |
29.00% |
5.90% |
6.90% |
19.40% |
35.30% |
37.90% |
12.90% |
|
Info. / News |
— |
3.40% |
— |
5.90% |
3.40% |
3.20% |
23.50% |
20.70% |
22.60% |
|
Adult content |
— |
— |
— |
— |
— |
— |
5.90% |
3.40% |
— |
|
Other |
— |
3.40% |
— |
— |
3.40% |
— |
— |
— |
3.20% |
|
Online shopping |
— |
— |
— |
— |
— |
— |
— |
— |
3.20% |
Internet Addiction Test (IAT)
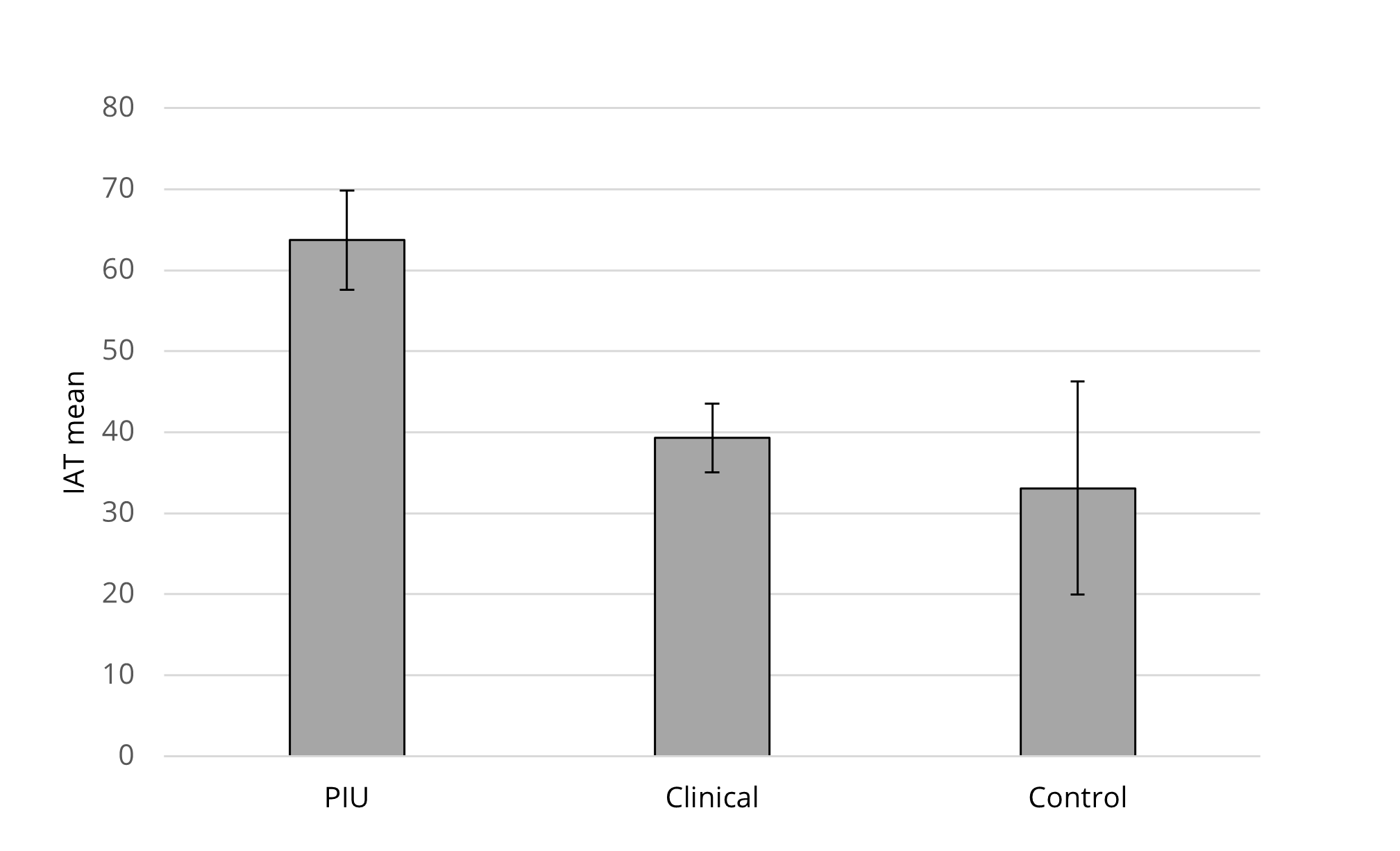
Results from the Internet Addiction Test (IAT) showed that the PIU group (M = 63.71, SD = 12.60) presented significantly higher Internet addiction scores than the clinical (M = 39.30, SD = 11.61, z = 30.64, p < .001) and the control (M = 33.09, SD = 6.57, Z = 41.49, p < .001) groups, c2kw(2) = 36.78, p < .001, h2 = .47. No significant differences were found between the clinical and the control groups (z = −10.85, p = .188).
Figure 1. Mean Comparison (With 95% CI Error Bars) for Internet Addiction Test (LAT)
Between the 3 Groups: Problematic Internet Use Group (PIU); Clinical Group; and Control Group.
Psychopathologic Evaluation
Beck Depression Inventory (BDI)
Results from the BDI showed that both the PIU group (M = 22.18, SD = 11.96, z = 36.06, p < .001) and the clinical group (M = 21.03, SD = 13.73, z = −32.23, p < .001) presented significantly higher depression scores than the control group (M = 3.31, SD = 4.48), c2kw(2) = 41.29, p < .001, h2 = .53. No significant differences were found between the PIU and the clinical groups (z = 3.83, p = .582).
Hospital Anxiety and Depression Scale (HADS)
Similar to the previous findings, results regarding depression showed that both the PIU group (M = 9.82, SD = 5.55, z = 33.05, p < .001) and the clinical group (M = 8.70, SD = 4.75, z = −30.28, p < .001) presented significantly higher depression scores than the control group (M = 2.00, SD = 2.72), c2kw(2) = 35.88, p < .001, h2 = .46. No significant differences were found between the PIU and the clinical groups (z = 2.78, p = .689).
Regarding anxiety, both the PIU group (M = 9.76, SD = 4.44, z = 23.31 p = .002) and the clinical group (M = 10.30, SD = 6.11, z = −23.54, p < .001) included significantly higher anxiety scores than the control group (M = 4.19, SD = 2.88), c2kw(2) = 19.99, p < .001, h2 = .26. No significant differences were found between the PIU and the clinical groups (z = −.23, p = .974).
Family Assessment Device—General Functioning (FAD-GF)
As for the family assessment, the results showed that both the PIU group (M = 2.47, SD = 0.73, p = .002) and the clinical group (M = 2.24, SD = 0.62, p < .01) presented significantly higher scores of problematic family functioning than the control group (M = 1.90, SD = 0.44), F(2) = 4.77, p = .002, η2 = .16. No significant differences were found between the PIU and the clinical groups (p = .757). Taking into consideration the threshold of 2.00 (Epstein et al., 1983), these results indicate that both PIU and clinical groups present problematic family functioning, contrary to the control group which showed a lower mean score.
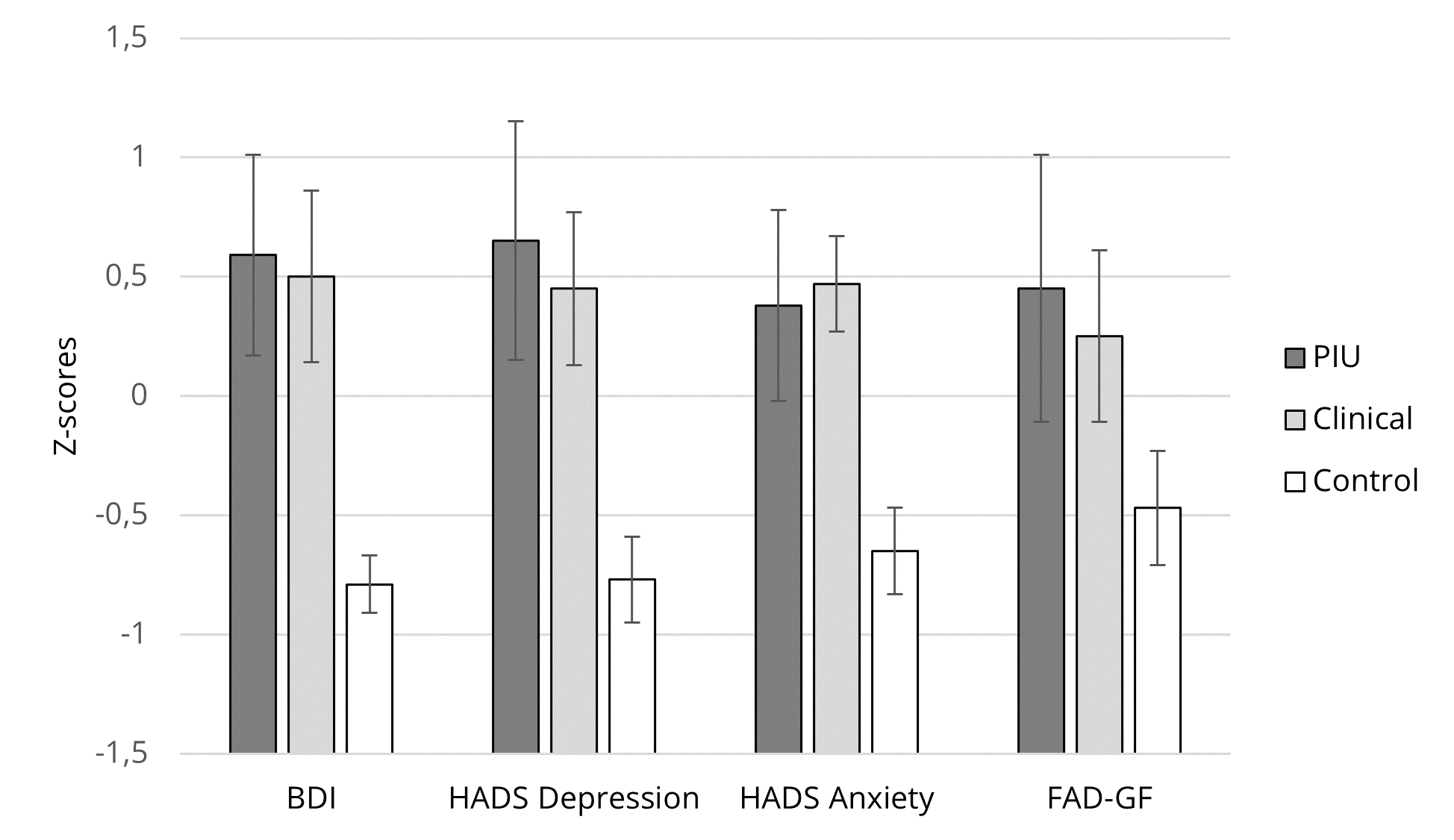
Figure 2. Mean Z-Scores Comparison (With 95% CI Error Bars) for Beck Depression Inventory (BDI),
Depression Subscale of the Hospital Anxiety and Depression Scale (HADS), Anxiety Subscale
of the HADS, and Family Assessment Device—General Functioning (FAD-GF) Between the 3 Groups:
Problematic Internet Use Group (PIU); Clinical Group; and Control Group.
Discussion
In favour of our first and second hypothesis, Problematic Internet Users seem to have other significant comorbid psychopathology beyond the expected dysfunctional Internet use (demonstrated through significantly higher scores in the IAT), calling into question the idea that PIU is a completely independent nosological entity—a seemingly pure entity disassociated from already known psychopathology. Our results support these hypothesis, which propose either an intermediate position for PIU in an angodepressive spectrum or an overlap (in which Problematic Internet Users have similar symptoms to the ones with diagnosed affective disorders).
Although Problematic Internet Users have higher IAT scores than the clinical group, we found no significant differences between these two groups regarding psychopathology, namely depressive symptoms measured by the BDI and the HADS, or anxiety symptoms measured by the HADS. Both PIU and clinical groups have similar and higher depression and anxiety levels than the control group, placing PIU as a new manifestation of already known affective disorders expressed and integrated into the era in which we live.
The idea that clinically relevant depressive and anxious symptomatology might be part of PIU features is supported by previous research that suggests that affective symptoms could be a cause and a consequence of PIU (Wu et al., 2016), especially depression (Tan et al., 2016; Zhong et al., 2011; Zhou et al., 2018). However, we find it highly relevant that the two groups in question (PIU and clinical) were collected from clinical populations, which were previously screened and evaluated as different. That is, the PIU group was collected from a clinical population diagnosed as having a PIU without other comorbid major symptoms, namely without a diagnosis of a depressive or anxious syndrome. We did not expect to find a total overlap, which suggests that these two groups may disclose overlapping affective symptoms in different presentations.
We speculated that the similitude between samples and yet such different clinical presentations could be explained if Internet acted as a buffer to affective psychopathology (Chou & Edge, 2012). We could speculate that PIU palliates several depressive symptoms and therefore masks usual symptoms of depressive disorder: for instance, offline anhedonia and self-devaluation hidden behind expressed pleasure and a notion of self-efficacy restricted to online activities, or isolation and insomnia masked by online exclusive relationships and voluntary inversion of the sleep-wake cycle. These findings warrant exploring the possibility of PIU as new (and generation biased) psychopathology of depressive or anxious states.
Our findings are supported by previous theoretical work: a model was initially described in which psychopathology predisposed an individual to maladaptive Internet cognitions which subsequently lead to the development of PIU (Davis, 2001). Later other authors (LaRose et al., 2003) applied Bandura’s theory (Bandura, 1991) of self-regulation and negative cognitive bias to explain depression as having a causal role in both motivating Internet overuse and generating problematic behavior. They theorized that depressed individuals are motivated to use the Internet to relieve under-stimulation and to access contents that will improve their affect. They also theorized that negative mood cognitively impairs depressed individuals’ ability to self-regulate their use, which leads to the development of PIU, suggesting that depression can both drive individuals to use the Internet and impair their ability to control their use (LaRose et al., 2003). This leads to a self-perpetuating cycle (Moreno et al., 2015).
The fact that our PIU sample presented depressive and anxious symptoms in BDI and HADS scales like those of clinical samples of affective disorders contrasts with the fact that none of these adolescents were signaled for psychiatric care. This suggest that core depressive and anxious symptoms might have different presentations and elude everyday clinical enquire. This would require devising new ways to clarify the symptoms.
Likewise, in our study, PIU and clinical groups presented significantly higher scores of problematic family function (measured by the FAD) than the control group and no significant differences were found between the PIU and the clinical groups. The control group had scores below the threshold that indicates a non-problematic family functioning. These results are in line with previous research showing that, similarly to anxious and depressed young people, Problematic Internet Users tend to have a scarcer perceived support network (in family, loving and friendship; Adiele & Olatokun, 2014; Durkee et al., 2012) and tend to live in poorly functioning families with less organized nuclear structures (mostly single-parent or rebuilt families of lower socioeconomic classes; Li et al., 2014; Wartberg et al., 2014; Wu et al., 2016; Zhong et al., 2011; Zhou et al., 2018), suggesting that family interventions could be a crucial element in the clinical approach to these patients. We also highlight the fact that most of the studied subjects admit depending on their family to access the Internet (that is, it is the family that pays for the supply). We believe that this result should be explored in future research focusing on the relationship between the family and PIU.
Finally, our results suggest that social networking only appears as a preferred activity for controls, while gaming appears only in those of the clinical groups. We could speculate that depressive subjects tend to use gaming as a coping mechanism that enhances pleasure, while healthy subjects engage in positive online social activities. Nevertheless, previous research has revealed mixed findings regarding the reciprocal associations between frequent technology use and psychological adjustment among adolescents. Examples are negative outcomes such as depressive symptoms (Eijnden et al., 2008), declines in subjective well-being (Kross et al., 2013) and the belief that others are happier (Chou & Edge, 2012); or positive outcomes such as increases in self-disclosure and friendship quality (Best et al., 2014; Valkenburg & Peter, 2009). This controversy has parallels with gaming since studies that emphasize benefits are also growing (Halbrook et al., 2019; Oing & Prescott, 2018).
Limitations
First our study should be considered exploratory as it includes a small sample. Due to its size, we cannot exclude type 1 or type 2 errors. The generalization of our results might be limited by the specifics of our sample as only one clinic was used. The construct of PIU is still heterogenous and under discussion, which might further determine the relevance of our results. Age and academic status showed differences across our sample groups, which seemed to be an artefact of the process of selection of the groups (age might be influenced by selection of the clinical group in an adolescent consultation where all patients must be 21 years old or less; education might be influenced by selection of the control group in a university hospital where all students have > 12th grade). Measures used in our study have (1) general limitations of self-reported instruments—understanding, under or overestimating of symptoms and Internet use and (2) further limitations of being used beyond their validation (e.g., Hamilton for depressive episodes). Follow-up data seem necessary to better necessary to better define the clinical relevance of PIU. Lastly, prescribed drugs and illicit substances were appraised and yet the small sample size did not allow the determination of their effect on our scores.
Conclusion
Our study suggests a positive association between depression and PIU for adolescents and young adults. This finding supports that among adolescents with depression screening for PIU could be warranted. Future work assessing the nature of Internet use in relation to the risk for PIU among individuals with moderate to severe depression may inform the development of specific treatment approaches and preventative guidelines for this population.
Conflict of Interest
The authors have no conflicts of interest to declare.

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Copyright © 2023 Cyberpsychology: Journal of Psychosocial Research on Cyberspace

